Stroke & Transient Ischemic Attack
Also known as:
Stroke – Cerebrovascular accident (CVA)
Transient Ischemic Attack – TIA or mini-stroke
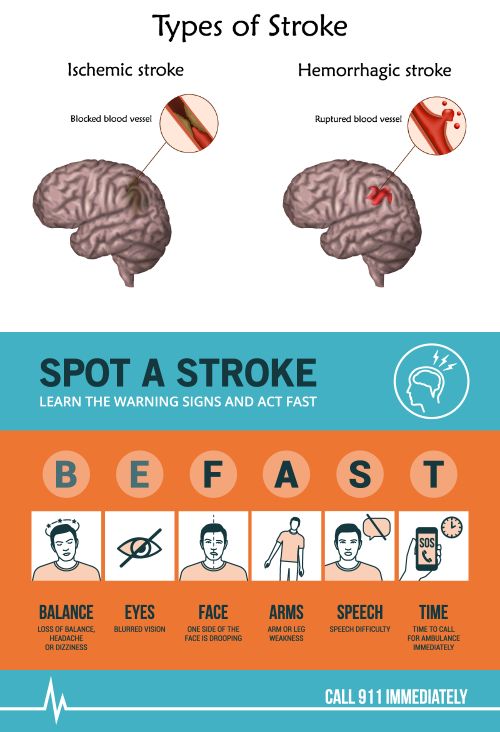
A stroke is caused when the blood flow to an area of your brain is blocked (ischemic) or when a blood vessel is ruptured (hemorrhagic). This leads to reduced blood flow downstream of the affected vessel which in turn cannot deliver oxygen and essential nutrients to the brain.
A stroke is a medical emergency and if the block continues for more than 3 to 4 minutes, it could lead to permanent brain damage and/or disability, hence the saying “time is brain.” This is the fifth leading cause of death in the United States.
Ischemic Stroke – usually occurs when the blood flow to the brain is blocked by a plaque or a clot. If the plaque and/or clot blocks one or more of the arteries in the brain, a transient ischemic attack or a complete stroke can occur.
Similar to a heart attack, over the course of time, inflammatory substances and cholesterol in the body build up in the artery walls forming atherosclerosis (also known as plaque). This gradually hardens and narrows the blood vessels.
If a piece of this plaque is broken off, a blood clot (thrombus) can be formed at the site of the break-off. Or a distant clot may also travel from the heart or other areas of the body and get stuck in the brain arteries.
- Transient Ischemic Attack (TIA) – also known as a mini-stroke, is a temporary loss of neurological function that can take place before a complete stroke. The symptoms can be similar to a stroke but they usually resolve in a few minutes or can last up to 24 hours.
Hemorrhagic – caused due to a rupture in a blood vessel and bleeding into the brain due to high blood pressure, weakness in the walls of the blood vessels, aneurysms, use of blood thinners, or trauma
- Subarachnoid Hemorrhage (most common)
- Parenchymal/Intracerebral Hemorrhage
- Intraventricular Hemorrhage

Note: Not everyone may experience all symptoms
- High blood pressure
- Smoking or the use of other tobacco products
- High LDL (bad cholesterol)
- Low HDL (good cholesterol)
- Pre-existing heart conditions
- Arrhythmias – especially Atrial Fibrillation
- Heart failure
- Heart infections
- Blood vessel malformations (AV malformations)
- Blood thinners
- Some birth control pills or hormone replacement therapy
- Pregnancy
- Stress
- Age – more common in older individuals
- Sex – more common in men and post-menopausal women
- Illicit drug use – cocaine
Show references
Boehme AK, Esenwa C, Elkind MS. Stroke Risk Factors, Genetics, and Prevention. Circ Res. 2017;120(3):472-495. doi:10.1161/CIRCRESAHA.116.308398
Steiger N, Cifu AS. Primary Prevention of Stroke. JAMA. 2016;316(6):658-659. doi:10.1001/jama.2016.5529
Hasan TF, Rabinstein AA, Middlebrooks EH, et al. Diagnosis and Management of Acute Ischemic Stroke. Mayo Clin Proc. 2018;93(4):523-538. doi:10.1016/j.mayocp.2018.02.013
Coutts SB. Diagnosis and Management of Transient Ischemic Attack. Continuum (Minneap Minn). 2017;23(1, Cerebrovascular Disease):82-92. doi:10.1212/CON.0000000000000424
Winstein CJ, Stein J, Arena R, et al. Guidelines for Adult Stroke Rehabilitation and Recovery: A Guideline for Healthcare Professionals From the American Heart Association/American Stroke Association [published correction appears in Stroke. 2017;48(2):e78] [published correction appears in Stroke. 2017 Dec;48(12 ):e369]. Stroke. 2016;47(6):e98-e169. doi:10.1161/STR.0000000000000098
